 Have you ever thought about the animals we use to test our medications on? The House Rabbit Society rescued two bunnies, Heather, and Lillian. They lived their entire lives in cages, never knowing what it was like to live outside of a laboratory. They did not know what hay or salad was and had never felt a loving hand pet them. They sustained injuries to their eyes and those injuries may never heal. Thanks to organizations like the
Have you ever thought about the animals we use to test our medications on? The House Rabbit Society rescued two bunnies, Heather, and Lillian. They lived their entire lives in cages, never knowing what it was like to live outside of a laboratory. They did not know what hay or salad was and had never felt a loving hand pet them. They sustained injuries to their eyes and those injuries may never heal. Thanks to organizations like the House Rabbit Society and the Beagle Freedom Project, animals are being saved from being poked and prodded all day for months at a time with no rest between tests. Scientists have created a new method for testing drugs. They developed organoids to help eliminate animal testing. Organoids are an artificially grown mass of cells, or tissue, that resembles an organ. Organoids go beyond the limitations of animal testing and are helping scientist recreate part of the body in vitro. Testing animals with medicines intended for human use does not provide accurate results and it is cruel to test on animals, leading scientists to create organoids, which have been discovered to be more accurate.
House Rabbit Society and the Beagle Freedom Project, animals are being saved from being poked and prodded all day for months at a time with no rest between tests. Scientists have created a new method for testing drugs. They developed organoids to help eliminate animal testing. Organoids are an artificially grown mass of cells, or tissue, that resembles an organ. Organoids go beyond the limitations of animal testing and are helping scientist recreate part of the body in vitro. Testing animals with medicines intended for human use does not provide accurate results and it is cruel to test on animals, leading scientists to create organoids, which have been discovered to be more accurate.
Scientist made organoids from the intestines first and have since made them from breast, liver, and brain cells. In the article, Organoids- the future of medical research, Louise Thompson said,” They are grown from stem cells, which has only become possible with the discovery of the precise conditions needed to keep stem cells alive outside the body.” Due to this discovery scientist will be able to better study diseases and how they develop in the organs. When scientists create organoids, they take cells from humans and create a mini three-dimensional organ that they can test medicines on. If someone had a disease and their cells were taken to create an organoid scientist could then test different medications on the organoid to see which one is best to help fight the disease. We could possibly have specialized drugs for each person using organoids.
Micro-organoids can overcome limitations that animals cannot. Christoph Giese stated in his Journal of Biotechnology, “Pharmaceutical drugs and compounds used for consumer products may bear the risk of unexpected immuno-toxicological side effects, such as sensitization, allergy, anaphylaxis or immunogenicity.” Scientist used the organoids in vitro to remodel lymphatic follicles, functional and structural cells along with lymphoid cells derived from peripheral blood mononuclear cells, which are cells with a round nucleus that help the immune system to fight infection and adapt to intruders, to produce a 3D tissue mimicking environment. The lymph node model was then used to show long term and repeated drug exposure to induce and monitor both cellular and humoral immune responses. Scientist could use the organoids to help them see how the drugs effected lymph nodes over the course of several weeks. According to the article Immunological Substance testing on Human Lymphatic Micro-organoids in Vitro, animal models do not reflect the complexity and the specificity of the human immune system sufficiently. Before we could configure this new method to test drugs, people were at risk because we could only guess how different the drugs would react between an animal and a human.
Not only are we unable to accurately compare the differences between humans’ and animal’s reaction to drugs, we are also unable to predict the long term affects. As Frank  Sonntag states, “It has been largely recognized that established substance safety testing in chemical, cosmetics and pharmaceutical sectors is poorly predictive to human long term exposure.” We knew we could not predict the long-term effects of how a drug would react to humans so we tried to find a more innovative way of testing drugs. According to the article Design and prototyping of a chip-based multi-micro-organoid culture system there’s a program called REACH funded by the U.S. National Toxicology program that’s in charge of enforcing the development of definitive predictive methods instead of animal testing. This program has helped push researchers to find new ways of testing drugs such as the organoid in vitro.
Sonntag states, “It has been largely recognized that established substance safety testing in chemical, cosmetics and pharmaceutical sectors is poorly predictive to human long term exposure.” We knew we could not predict the long-term effects of how a drug would react to humans so we tried to find a more innovative way of testing drugs. According to the article Design and prototyping of a chip-based multi-micro-organoid culture system there’s a program called REACH funded by the U.S. National Toxicology program that’s in charge of enforcing the development of definitive predictive methods instead of animal testing. This program has helped push researchers to find new ways of testing drugs such as the organoid in vitro.
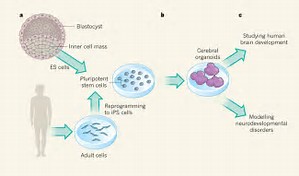
Scientists have been able to develop parts of the body using organoids. The brain is so  complex it has made it hard to study brain disorders using model organisms, increasing the need for in vitro models of the brains development. According to Madeline Lancaster an author from the article, Cerebral organoids model human brain development and microcephaly “Finally, we use RNA interference and patient-specific induced pluripotent stem cells to model microcephaly, a disorder that has been difficult to recapitulate in mice. We demonstrate premature neuronal differentiation inpatient organoids, a defect that could help to explain the disease phenotype.” She also goes on to say,” Together, this data shows that three-dimensional organoids can recapitulate development and disease even in the most complex human tissue.” Without the development of organoids, we would still be using mice to try and recapitulate microcephaly and we would not be any closer to getting results that would help us find a cure for the disease. Testing on animals served its purpose in the late 1930s but now we need to stop using animals to help find cures for diseases and use in vitro testing. Not only have we created mini brains to study but scientists at Columbia University created lung organoids to mimic features of full-sized lungs to help us have a better understanding of respiratory diseases. Hans-Willem Snoeck, a professor of medicine at Columbia University Medical Center, said in a press release,” Organoids, created with human pluripotent or genome-edited embryonic stem cells, may be the best, and perhaps only, way to gain insight into the pathogenesis of these diseases.” Being able to use the patients cells to create a mini organ with the same disease will help scientist be able to study the disease better. Researchers show the organoids react the same way a real lung reacts when infected with Respiratory syncytial virus and when they have a gene mutation linked to pulmonary fibrosis. Being able to replicate an infection or disease in any part of the body will help us learn and understand how the disease/ infection works and what medications will best help get rid of the infection and help find a cure for diseases.
complex it has made it hard to study brain disorders using model organisms, increasing the need for in vitro models of the brains development. According to Madeline Lancaster an author from the article, Cerebral organoids model human brain development and microcephaly “Finally, we use RNA interference and patient-specific induced pluripotent stem cells to model microcephaly, a disorder that has been difficult to recapitulate in mice. We demonstrate premature neuronal differentiation inpatient organoids, a defect that could help to explain the disease phenotype.” She also goes on to say,” Together, this data shows that three-dimensional organoids can recapitulate development and disease even in the most complex human tissue.” Without the development of organoids, we would still be using mice to try and recapitulate microcephaly and we would not be any closer to getting results that would help us find a cure for the disease. Testing on animals served its purpose in the late 1930s but now we need to stop using animals to help find cures for diseases and use in vitro testing. Not only have we created mini brains to study but scientists at Columbia University created lung organoids to mimic features of full-sized lungs to help us have a better understanding of respiratory diseases. Hans-Willem Snoeck, a professor of medicine at Columbia University Medical Center, said in a press release,” Organoids, created with human pluripotent or genome-edited embryonic stem cells, may be the best, and perhaps only, way to gain insight into the pathogenesis of these diseases.” Being able to use the patients cells to create a mini organ with the same disease will help scientist be able to study the disease better. Researchers show the organoids react the same way a real lung reacts when infected with Respiratory syncytial virus and when they have a gene mutation linked to pulmonary fibrosis. Being able to replicate an infection or disease in any part of the body will help us learn and understand how the disease/ infection works and what medications will best help get rid of the infection and help find a cure for diseases.
When we create organoids, we take cells from a patient and use them to make a mini model of the patient’s liver, kidney, brain, intestines, and other organs. Since we’re using the patient’s own cells Madeline Lancaster said in the article, Organogenesis in a dish: modeling development and disease using organoid technologies,” Tissues derived in vitro could be generated from patient cells to provide alternative organ replacement strategies. Unlike current organ transplant treatments, such autologous tissues would not suffer from issues of immunocompetency and rejection.” This development could not only help cut down the use of animals in laboratories but also help save people who are on the transplant list waiting for a match. We would not be able to recreate organs and hopefully use them in place of putting people on a transplant lists if we still relied on animal testing. Science is advancing so fast and we need to advance with it and get rid of the things that are not contributing to the growth of a new generation of science.
In 1937, a pharmaceutical company created a drug to treat streptococcal infections. The chemist used a solvent called diethylene glycol and added raspberry flavoring and sold it as Elixir Sulfanilamide. This medicine was the cause of more than a hundred deaths because diethylene glycol is poisonous to humans. In the article, Animal Testing: A Long, Unpretty History, wrote by Susan Scutti she says, “The public outcry caused by this incident and similar disasters led to the passing of the 1938 Federal Food, Drug, and Cosmetic Art requiring safety testing of drugs on animals before they could be marketed.” In 1938, we needed to find a way to test drugs so we could try to prevent another catastrophic like the one in 1937 from happening. Testing animals for medications and cosmetics can leave permanent damage to the animals. To try and find cures for patients with potentially fatal diseases we first must give the animal the disease. We are giving animals cancer and aids to try and find cures for humans but the drugs that cured the animals of the diseases were not effective on humans. In the 1950s the sleeping pill thalidomide caused 10,000 babies to be born with severe deformities. The drug was tested on pregnant mice, rats, guinea pigs, cats, and hamsters. The babies did not have birth defects unless the pregnant moms were given an extremely high dose.
 Animal testing might have been necessary in 1938, but science has evolved since then and we have more innovative research to help us test the toxicology of drugs and the long-term effects they have on humans. Even if we had not discovered organoids we would not be able to rely on the results we get from testing medications on animals. Not only is testing on animals cruel it is also unhelpful. Scientists become so consumed with trying to find cures for the diseases they inject in the animals that they forget our bodies are physiologically different than animals. Research has changed so much since 2010 when scientist first started to create organoids. The innovative research scientists have come up with in the past 7 years is making the need for animal studies to decline. We will soon be able to stop giving animals cancer and aids because the organoids are helping us find better medications faster.
Animal testing might have been necessary in 1938, but science has evolved since then and we have more innovative research to help us test the toxicology of drugs and the long-term effects they have on humans. Even if we had not discovered organoids we would not be able to rely on the results we get from testing medications on animals. Not only is testing on animals cruel it is also unhelpful. Scientists become so consumed with trying to find cures for the diseases they inject in the animals that they forget our bodies are physiologically different than animals. Research has changed so much since 2010 when scientist first started to create organoids. The innovative research scientists have come up with in the past 7 years is making the need for animal studies to decline. We will soon be able to stop giving animals cancer and aids because the organoids are helping us find better medications faster.
We have also began using organoids to streamline the drug discovery process for head and neck cancer. Due to high toxicities from chemotherapy, surgery, and radiation therapy the patients are getting damage to their tissues and organs that are anatomical sites critical for breathing, eating and talking. Preserving the patient’s3+ tissues and organs is very important so they can maintain normal function. “In Vitro three-dimensional cultures grown from primary tumor tissue (organoids) are attractive for a high-throughput drug screen that enables testing of multiple drugs and drug combinations. Cellular level measurements can identify cell subpopulations that exhibit different sensitivities to treatments, and organoids combined with high-resolution imaging of cell metabolism provides a promising platform.” According to Amy Shah professor in the Department of Biomedical Engineering at Vanderbilt University. Since the organoids are created from the tumor tissue we can capture distinct behaviors of individual tumors. (Shah et al). A big problem with trying to find new medications for cancer patients is it takes at least ten years to develop a drug and can cost over one billion dollars to fund. Organoids could allow us to test the drugs a lot quicker and maybe cost less money. Being able to test drugs on the in vitro organs with tumor tissue would allow us to see how they react to the drug treatments. Seeing how the organoids react would then help us develop a form of therapy that has a higher efficacy and lower toxicity. This study is solely focused on patients with head and neck cancer but the same things are being done for other diseases.
We all know testing on animals is not right so why do we still rationalize the need for animal testing? Organoids go beyond the limitations of animal testing and are helping scientist recreate part of the body in vitro. Testing animals with medicines intended for human use does not provide accurate results, leading scientists to create organoids, which have been discovered to be more accurate. Scientists are evolving the way they test medications and are finding the need to test on animals is not as apparent as before. We need to reduce the use of animals and eventually stop the use of animals in medical experiments, reduce the number of animals tested on every year, and refine the way we allow experiments to be carried out. We need to embrace the change from testing on animals to testing on organoids.
Works Cited
Giese, Christoph, Annika Lubitz, Christian Demmler, Jana Reuschel, Konstanze Bergner, and Uwe Marx. “Immunological Substance Testing on Human Lymphatic Micro-organoids in Vitro.” Immunological Substance Testing on Human Lymphatic Micro-organoids in Vitro. N.p., n.d. Web. 08 May 2017.
Lancaster, Madeline A., Magdalena Renner, Carol-Anne Martin, Daniel Wenzel, Louise S. Bicknell, Matthew E. Hurles, Tessa Homfray, Josef M. Penninger, Andrew P. Jackson, and Juergen A. Knoblich. “Cerebral Organoids Model Human Brain Development and Microcephaly.” Nature News. Nature Publishing Group, 28 Aug. 2013. Web. 08 May 2017.
Lancaster, Madeline A., and Juergen A. Knoblich. “Organogenesis in a Dish: Modeling Development and Disease Using Organoid Technologies.” Science. American Association for the Advancement of Science, 18 July 2014. Web. 08 May 2017.
Mattei, Giorgio, et al. “On the Adhesion-Cohesion Balance and Oxygen Consumption Characteristics of Liver Organoids.” Plos ONE, vol. 12, no. 3, 07 Mar. 2017, pp. 1-19. EBSCOhost, doi:10.1371/journal.pone.0173206.
Ping, Wang, et al. “CRISPR/Cas9-Mediated Heterozygous Knockout of the Autism Gene CHD8 and Characterization of Its Transcriptional Networks in Cerebral Organoids Derived from Ips Cells.” Molecular Autism, vol. 8, 20 Mar. 2017, pp. 1-17. EBSCOhost, doi:10.1186/s13229-017-0124-1.
Shah, Amy T., et al. “Metabolic Imaging of Head and Neck Cancer Organoids.” Plos ONE, vol. 12, no. 1, 18 Jan. 2017, pp. 1-17. EBSCOhost, doi:10.1371/journal.pone.0170415.
Sonntag, Frank, Niels Schilling, Katja Mader, Mathias Gruchow, Udo Klotzbach, Gerd Lindner, Reyk Horland, and Ilka Wagner. “Design and Prototyping of a Chip-based Multi-micro-organoid Culture System for Substance Testing, Predictive to Human (substance) Exposure.” Design and Prototyping of a Chip-based Multi-micro-organoid Culture System for Substance Testing, Predictive to Human (substance) Exposure. N.p., n.d. Web. 08 May 2017.

Learned something new and cool. Great job with the background section.
LikeLike