Society dictates of how beauty should be defined when it comes to how proportionate the person’s facial features are as it fits the golden ratio, and more importantly, how flawless a person’s skin has as visibly seen by the eyes of the beholder. Nevertheless, the skin is the first line of defense when it comes to protecting the body from external harsh environment. Skin problems and illnesses are frequently noticeable and visible to others that even a physician can generally diagnose what a person has by looking at the abnormal skin level. The social stigma customarily correlated with different types of skin conditions is hard for people to cope with their skin issues and diseases, as well as negative reaction they receive from others. Moreover, many people suffer from variety of skin problems whether it is hereditary, autoimmune, infectious, environmental, or of unknown cause. Thus, it is the goal of this paper to look into a deeper understanding of one of the prevalent skin diseases, such as psoriasis, though untreatable, yet can be prevented as long as the underlying causes are known intracellularly and externally.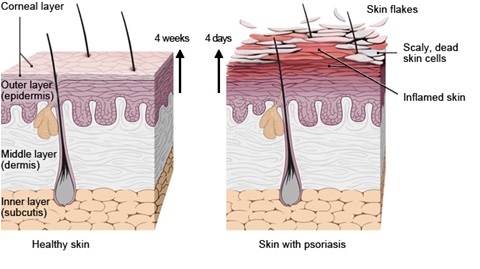
Fig. 1. Healthy skin and skin with psoriasis. “Growth and Shedding of Keratinocytes in Psoriasis.”Psoriasis Plaque, PubMed Health, https://www.ncbi.nlm.nih.gov/pubmedhealth/PMHT0030407/
Normally, the skin regenerates itself about once a month, or approximately every twenty-eight days (Pagano 18) or 4 weeks as shown in Fig. 1 in a healthy skin (Growth and Shedding of Keratinocytes in Psoriasis). However, in psoriasis, the process speeded up; the skin attempts to renew itself every three or four days instead of the twenty-eight days. The surface area becomes red, inflamed, extremely sensitive, visibly raised, and scaly (19).
The word psoriasis is from the Greek word psora, which means “itch” (Raychaudhuri et al. 61). Psoriasis is a long term, immune-mediated inflammatory disease (IMID , a disease that lacks definitive etiology) that occurs from the hyperproliferation of skin cells, thus thickening the layer of skin, which causes erythema or redness, scaly silvery plaques, itching, and bleeding. It is genetically inherited from a mother or father who has the disease. Psoriasis is not an unusual disorder; a prevalence of 2%-4%, with a peak incidence between 15 and 25 years age and without sex predilection, has been reported (45).
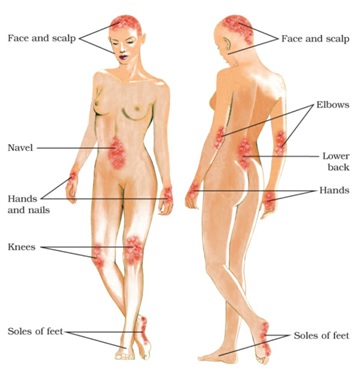
Fig. 2. Common affected areas in psoriasis. “Main Features of Psoriasis.”Psoriasis E-Chart.HC-HealthComm, loc. 63, http://www.hc-healthcomm.com
The manifestation of psoriasis can be triggered by many factors. It can be triggered by external and internal environmental factors in genetically susceptible individuals. These factors include infections, drugs such as allergic drug reaction, antimalarial drugs, lithium, beta blockers, interferon alpha, withdrawal of systemic corticosteroids, local trauma (Koebner’s phenomenon), and emotional stress, as these correlates with the onset or flares of psoriatic lesions (Weinberg 11). These lesions are distributed symmetrically and frequently occur on the elbows, knees, lower back, and scalp. These plaques can be intensely pruritic and bleed when manipulated, referred to as Auspitz sign (12). Thus, emotional stress, drugs, and infections can trigger clinical signs and symptoms experienced by psoriatics such as itching, bleeding, and lesion at the more prominent body sites such as the knees, elbows, back, and scalp as shown in fig. 2.

Fig. 3. Pathophysiology of psoriasis at a cellular level. “Evolution of Psoriasis and Immune Factors.” Psoriasis E-Chart.HC-HealthComm, loc. 51, http://www.hc-healthcomm.com
In many diseases that most people suffer, it seemed psychological distress plays a huge role in the exacerbation of the disease. Doctors and many people believe psychological ‘stress’ to be a major triggering factor in many skin diseases, specifically psoriasis (Shuster 614). The correlation between skin and mind may be a result of the skin’s role as biological structure of transmitting information, and perhaps also the social response to the infectious nature of skin disease in the recent past; consequently a disorder of the skin may have a very severe effect on the mind (615). He infer this is the basis of the erroneous belief that mind is a significant etiological aspect in skin disease. Moreover, he believes that there is a strong proof that both mind and ‘stress’ transform certain skin circulatory and immune responses but in a direction which might be anticipated to improve psoriasis (615). Therefore, based on the belief by many expertise in the field of medicine, psychological stress can worsen psoriasis.
There are many cases have been reported that stress can exacerbate psoriasis. Scientific research reports roughly 40% of cases in the beginning or worsening of psoriasis, psychosocial stress has been reported to play an important role (Gupta et al. 166). A few studies have been published that about 80% of patients with psoriasis are stress reactors. Many psychosocial intercessions have been reported to be a vital addition in the typical therapeutic management of psoriasis (166). Based on the study of 127 patients with plaque psoriasis who got admitted to Dermatology inpatient unit, the psychosocial stress measures such as major life events, psychological or personality factors, social support, and minor daily stressful events or hassles were used to evaluate the severity of the disease of psoriatic patients (168). Based on the result of the dermatologic measures that were done, it revealed that the high stress reactors (i.e. stress exacerbates psoriasis) had extensive psoriasis on head (face and scalp), neck, upper extremities, and genital area which are classified as “emotionally charged” because psoriasis in these anatomical parts are more likely to induce emotional reactions in the patients … In retroactive study, the high stress reactors also reported a larger number of flare-ups of their psoriasis during the 6 months prior to admission (170). In this study, the psychocutaneous traits have identified the high stress reactors from the low stress reactors (i.e. less significant link of stress and psoriasis). The high stress reactors had more disfiguring psoriasis because it affected many regions of their body.
Aside from what Gupta and his colleagues had mentioned above, another scientific study suggests that stress can cause psoriasis. Based on Al’Abadie et al research on the effects of stressful life events on the beginning and progress of psoriasis, their studies showed that psoriasis patients’ disease is affected by stressful events differing from 40 to 80% based on whether it is an acute or chronic stress, and based on patients self reports or responses based on standardized check-lists (199). They also added that stress can affect the immune system directly through neuroendocrine changes or indirectly through poor healthy habits in regards to diet and sleep, or by taking drugs such as alcohol and therefore lowering their immune system (199). They found that chronic stress of everyday struggles can worsen psoriasis (200). The results of the study supports that the experience of stress may take a significant part in the onset and exacerbation of psoriasis.
Many credible researchers continue to emphasize stress as one of the causes of the progression of psoriasis. In the study performed by Griffiths and Richards, they stated that psoriasis suggested as a psychosomatic disorder wherein stress or psychological distress is a cause in expressing the disease. Also, in their article, “Psychological influences in Psoriasis,” emotional stress was mentioned as the most convincing precipitating factor in psoriasis (338). The result of their study reported over 60% of a sample of psoriasis patients who attended a specialty clinic were convinced that stress was the main reason to the cause of their psoriasis, and this was not related to the clinical severity of their condition as measured by the Psoriasis Area Severity Index (PASI) (338). In addition, they also examined the Psoriasis Life Stress Inventory (PLSI) which is another way in rating everyday life struggles or recurring substandard stress associated with having to live with psoriasis. They were able to identify that the two main factors to stress in psoriasis were “engaging in anticipatory and avoidance coping behavior, and belief of being evaluated on the basis of their skin” (qtd 339). Furthermore, they deduce that if psoriasis patients engage themselves in anticipatory and avoidance coping behavior which is not related to their skin condition, then it might be hypothesized that “thoughts related to stigmatization and rejection may be influencing such behavior” (qtd 339). In other terms, psoriasis patients are expecting horrible situation when they are not aware that this will actually happen. One good example would be a psoriasis patient will not take her children to a public water park for fear of being asked to leave the premise due to the fact that they have psoriasis even though this might never have occurred to them in the past. They tried to avoid this kind of situation because they feel being stigmatized because of the clinical condition of their skin. Therefore, emotional or psychological stress of daily struggles with psoriasis manifests the progression of the disease.

Fig. 4. Commonly affected areas of psoriasis and types of treatment. Armstrong, April W. “Psoriasis is a Common Condition Where the Skin Gets Red and Scaly; Psoriasis can Cause Itching, Discomfort, and Sometimes pain.” JAMA Dermatology, vol. 153, no. 9, Sep. 2017, p. 956.
There are different types of treatment for psoriasis (see fig. 4). It can be topical medication, phototherapy, biological agents, oral medication, and diet. Though psoriasis can be stress related, having psoriasis self-help groups and group therapy that help the psoriatic patients to deal with the daily stresses related with their disease should be part of the whole therapeutic programs (Gupta et al. 172). The dermatologist should tailor the treatment plan based on patient individual needs since everybody has different and unique biochemical makeup. Though there is no cure for psoriasis, all the possible treatment mentioned above can possibly prevent the onset and exacerbation of the disease.
Topical medications are used to treat the symptoms of psoriasis. Salicylic acid, corticosteroids and vitamin D analogues are few of the topical agents used to alleviate the symptoms of psoriasis. Raychaudhuri states that due to increased water loss and increased formation of keratinocytes in the skin, the skin becomes dry and itchy (246). Salicylic acid emollients are applied on the psoriatic skin to moisten the epidermal layer and prevent it from pruritus or itching (246). On the other hand, inflammation of the skin is another symptoms experienced by psoriatic patients. Since psoriasis can be an autoimmune disease, the keratinocytes in psoriasis are not well regulated causing an inflammatory response. Vitamin D has many important roles in immunity and the absorption of calcium according to Fett (163). Vitamin D supplement added in diet of psoriasis patients has a moderate or greater improvement in psoriasis in at least 50 percent of patients in five separate studies that have been reported (164). Some psoriatic patients who take higher doses of vitamin D supplements completely resolved their disease (164). Vitamin D analogues are used to strengthen the immune system, and it binds to intracellular vitamin D receptors to regulate the genes responsible in the proliferation of keratinocytes and keratin (Raychaudhuri 249-50). The same effect as vitamin D ointment happens when corticosteroid is used to treat inflammation in psoriasis. Corticosteroid, a steroid hormone, is produced in the adrenal cortex regulates inflammatory response. It attaches to glucocorticoid receptor in the cell and regulates the gene responsible in inflammation (248). Therefore, the symptoms of psoriasis such as itching and inflammation can be treated with salicylic acid, vitamin D compounds, and corticosteroid topical agents.
Another treatment used to relieve the symptom of psoriasis is by the use of phototherapy. Ultraviolet (UV) light therapy is used as a phototherapy to slow the growth of the affected skin cells in psoriasis (Raychaudhuri 170). Since psoriasis is a T cell mediated disease, the abnormal functioning T lymphocytes attacks the skin cells causing an inflammatory response by increasing the keratinocyte proliferation and keratinization (Dolgin 1219). Thus, with phototherapy, it slows down the process of the T lymphocytes in attacking the keratinocytes.
Aside from the topical agents and phototherapy, diet also plays a vital role in the treatment of psoriasis. It is very essential to maintain the proper pH balance in the chemistry of psoriasis patients. Diet assists in the maintenance of a proper acid-base homeostasis of the chemical activity in the body according to Pagano (71). He suggests that psoriatic patients should be on the basic (alkaline) side than the acidic side as nature demands. The body chemistry that is leaning more towards the alkaline is more resistant to all kinds of disease (71). Furthermore, he recommends eating alkaline-forming foods such as raw carrot, celery, beets, parsley, romaine, lettuce, and spinach juice extracts, and avoids acid-forming foods such as strawberries, citrus fruits, citrus juices, and avocados (73-75). He mentions that a person’s blood should be always on the slight alkaline side (pH 7.3-7.5) to maintain the ideal health and immunity (71). Therefore, psoriatic patients should be aware of their diet to maintain alkalinity in the blood and body chemistry to have a better resistance to disease and strengthen their immunity.
Psoriasis is a very serious disease when it comes to the personal well being of a person who suffers from it. Knowing the possible stressors of psoriasis can help psoriatic patient treat its symptoms before its onset and exacerbation. Though the exact cause of psoriasis is unknown, bacterial or viral infections, toxic drugs, and psychosocial distress are few possible stressors of psoriasis. These stressors can cause the skin cell to behave erratically causing itchiness and inflammation of the skin. Many clinical studies have suggested that psychosocial stress can cause the exacerbation of psoriasis. Furthermore, a good mental attitude towards the disease is important to look at because they need a strong support group as they live their life daily with all the struggles they experience with the disease. In addition, different types of treatments such as topical agents (salicylic acid, vitamin D compounds, and corticosteroids), phototherapy (ultraviolet light), and diet are used to treat itching, inflammation, and other symptoms of psoriasis. Diet plays a very important role in alleviating the symptoms of psoriasis as long as the body chemical atmosphere is within the alkaline side for it aids a person from being resistant to diseases and increase its immunity. A deeper understanding of the stressors of psoriasis can help many people to win their battle with psoriasis.
Works Cited
Al’ Abadie, M. S. et al. “The Relationship Between Stress and the Onset and Exacerbation of Psoriasis and Other Skin Conditions.” British Journal of Dermatology, no. 130, 1994, pp. 199-200.
The article discusses the relationship between stress and beginning and progression of psoriasis. Dr. Mohammed Sami Al’ Abadie has worked in Dermatology since 1989, obtaining his PhD in Dermatology from Sheffield University, DSBD Diploma in Dermatology from University of Wales, working as a consultant Dermatologist since 1997. He is also a senior lecturer and visiting professor of medical students from Birmingham University, and has published numerous specialist papers in peer review journals in Dermatology. The article is important to utilize in the research paper due to one possible cause of psoriasis is stress.
Armstrong, April W. “Psoriasis is a Common Condition Where the Skin Gets Red and Scaly; Psoriasis can Cause Itching, Discomfort, and Sometimes pain.” JAMA Dermatology, vol. 153, no. 9, Sep. 2017, p. 956.
The article talks about common symptoms experienced by psoriatic patients. Dr. April W. Armstrong is an Associate Dean of Clinical Research at Keck School of Medicine at USC. She also serves as Director of Clinical Research for the Southern California Clinical and Translational Research Institute. In the Department of Dermatology at USC, she serves as Vice Chair, Director of Clinical Trials and Outcomes Research, and Director of the Psoriasis Program. The article is very useful in knowing the symptoms of psoriasis.
“Evolution of Psoriasis and Immune Factors.” Psoriasis E-Chart.HC-HealthComm, loc. 51, http://www.hc-healthcomm.com
The article accounts for the pathophysiology of psoriasis and anatomical areas affected by psoriasis. The information provided by this article can be helpful in knowing what really is going on at the cellular level in psoriasis.
Fett, Rebecca. Healing Arthritis and Psoriasis by Restoring the Microbiome: The Keystone Approach. Franklin Fox Publishing, 2018, pp. 163-164.
The author helps us understand the root causes of the autoimmune diseases, for instance, the psoriasis. She affirms, based on scientific research, that the balance of bacteria in an individual’s microbiome can have a huge impact on inflammation throughout the body. She also reveals the importance of a low-starch and microbiome-restoring diets for people who are suffering psoriasis. The author is a science writer with a degree in molecular biotechnology and biochemistry from the University of Sydney. She previously spent ten years as a biotechnology patent litigation attorney in New York, where she specialized in analyzing the scientific and clinical evidence for immune-targeting biologic medicines. I will use this source to support my research paper regarding the connection or roll of diets in psoriasis.
Griffiths, C. E., and Richards, H. L. “Psychological Influences in Psoriasis.” Clinical and Experimental Dermatology, no. 26, 2001, pp. 338-339.
The article explains how patients with psoriasis experience psychosocial activities like high anxiety level, depression, worry and avoidance of social activities. It also suggests that one of the main sources of stress experienced by patients with the said skin condition is due to apprehension of how others will react to their disease, which leads to avoidance behavior and extreme worrying. C. E. M. Griffiths OBE (Order of the British Empire) is Foundation Professor of Dermatology at the University of Manchester, Director of the Manchester Centre for Dermatology Research and Head of the Dermatology Theme of the National Institute for Health Research Manchester Biomedical Research Centre. He is also an Honorary Consultant Dermatologist at Salford Royal NHS Foundation Trust. On the other hand, H. L. Richards of Mercy University Hospital, Cork is also a researcher with an expertise in Positive Psychology, Health Psychology, and Clinical Psychology. I will use this source to get more information between the relationship of psoriasis and stress.
“Growth and Shedding of Keratinocytes in Psoriasis.”Psoriasis Plaque, PubMed Health, https://www.ncbi.nlm.nih.gov/pubmedhealth/PMHT0030407/
Gupta, Madhulika A. et al. “A Psychocutaneous Profile of Psoriasis Patients Who Are Stress Reactors: A Study of 127 Patients.” General Hospital Psychiatry, vol. 11, no. 3, May 1989, pp. 166-173. PubMed, http://dx.doi.org/10.1016/0163-8343(89)90036-4.
Gupta and his colleagues have identified some psychocutaneous distinctiveness that clinically differentiates psoriatirc who report that stress aggravates their disease (high stress reactors) from the psoriatics who do not report a considerable relationship between stress and their psoriasis (low stress reactors). The high stress reactors have more distorting illness as result of severe psoriatic flare ups in “emotionally charged” body parts. Madhulika Gupta is a scientist and affiliated at Division of Maternal, Fetal & Newborn Health, Children’s Health Research Institute, and assistant Professor in the Department of Paediatrics and Biochemistry in the Schulich School of Medicine & Dentistry in Western University. She is a very credible author that I can utilize in my research as it relates to the stressor of psychosocial influence to the exacerbation of psoriasis.
“Main Features of Psoriasis.”Psoriasis E-Chart.HC-HealthComm, loc. 63, http://www.hc- healthcomm.com
Pagano, John O. A., D.C. Healing Psoriasis: The Natural Alternative. John Wiley & Sons, 2009, pp. 18-19, 71, 73-75.
Dr. John Pagano defines in his book what is psoriasis and its etiology. He discusses the importance of diet and mental attitude in overcoming psoriasis. He also reveals how acid-forming diet, stress and any negative emotions such as hatred, anger, fear and the likes can aggravate the psoriatic condition. The author is a chiropractic physician in Englewood Cliffs, New Jersey, for forty eight years. His motivation to conduct research on and study psoriasis is due to His first encounter with his psoriasis patients while doing his internship at a hospital in Denver has motivated him to conduct research on psoriasis to alleviate the suffering of the people with the said disease. He wants to prove that psoriasis and other skin problems or diseases can be controlled and healed naturally. I strongly believe that the author is a reliable source and his book will be able to help me on my research paper to validate some claims and answer questions regarding the causes of psoriasis, and how it can be treated.
Raychaudhuri, Siba P. et al. Psoriasis and Psoriatic Arthritis: Pathophysiology, Therapeutic
Intervention, and Complementary Medicine. Taylor & Francis Group, 2018, pp. 37, 61, 170, 246, 248-250.
The authors present information on pathophysiology, disease epidemiology, and genetics of psoriasis and psoriatic arthritis. They cover the current treatments for psoriasis and psoriatic arthritis, which includes topical preparations, light therapy, and the idea of total care. In addition, they discuss the numerous nutriceutical supplements and functional foods available for psoriasis and its accompanying inflammatory conditions. Siba P. Raychudhuri, MD, FACP, FACR, is the chief of the Rheumatology Division at the VA Medical Center in Sacramento, California, and a senior faculty in the Division of Rheumatology, Allergy and Clinical Immunology at the University of California, Davis. Smriti K. Raychaudhuri, MD, is a professor of medicine and medical microbiology at California Northstate University College of Medicine. She is also the director of the Cellular and Clinical Immunology Research Laboratory at the Sacramento VA Medical Center, California. Lastly, Debasis Bagchi, PhD, MACN, CNS, MAIChE, is the chief scientific officer at Cepham Research Center, Piscataway, New Jersey; a professor in the Department of Phamacological and Pharmaceutical Sciences at the University of Houston College of Pharmacy, Texas. I will use this source to explain the pathophysiology of the disease process of psoriasis.
Shuster, Sam. “Stress and Psoriasis.” British Journal of Dermvatology. vol. 100, no. 5, 1979.
pp. 614-615.
The article discusses the relationship of stress and psoriasis. Dr. Sam Shuster is a British dermatology educator, consultant, and researcher. He is an honorary consultant at Norfolk and Norwich University Hospital since 2009. Consultant on various pharmacological and chemical industries worldwide, television and radio programs on medical and general topics. The article provides information about how stress affects psoriasis.
Weinberg, Jeffrey M. Treatment of Psoriasis. Birkhauser, 2008, p. 11.
The book expounds the pathopysiology of psoriasis and the triggering factors of it. The author describes, as well, the different types of psoriasis like erythrodermic psoriasis, pustular psoriasis, inverse psoriasis, nail psoriasis, oral psoriasis, and psoriatic arthritis. He also discusses the different ways to treat psoriasis- oral therapy, topical therapy, UV and laser therapy. Furthermore, he points out some medications that can trigger psoriasis. The author is a Dermatology specialist in Forest Hill, New York. He attended and graduated from University of Pennsylvania School of Medicine in 1993. This book will be helpful to fully understand the disease process and treatments
