There were 69,000 troops recruited into the armed forces last year. When veterans come home a percentage have long-term effects that haunt them daily and need to be treated by medical specialists. These issues include PTSD, depression and anxiety that make it hard to function as a civilian and lead to significant health problems. Many struggle to acclimate back into society with mental and physical issues that need to be addressed and treated. Studies regarding PTSD and sleep disturbances veterans experience and some treatments available for the issue, the effects for both the veteran and their families with quality of life as well as their relationships.

Insomnia may be the most common among veterans with a complaint of sleep issues. Mood and anxiety result in lack of sleep with other psychological effects. Some can fall asleep but can’t stay asleep due to nightmares or just have difficulty falling asleep. In a study done my van -Liempt (470-471), shows the demographics of veteran involved and the issues they develop after being discharged. Other factors may play a part in how anxiety or stress levels but mainly due to PTSD disrupted sleep. Pre-deployment anxiety symptoms increase the risk in developing PTSD symptoms although all remain negatively affected. If REM sleep is disturbed or fragmented, nightmares may be triggered due to PTSD and lack of rest creating mental and physical distress. It may contribute directly to the development of PTSD disrupting the beneficial process of sleep on fear distinction. Those with nightmares may talk, scream or physically move and disturb their partner or create a hostile sleeping situation. Exhaustion may result in lack of sleep creating strain on relationships and personal life impacted and seclusion for the severely disturbed.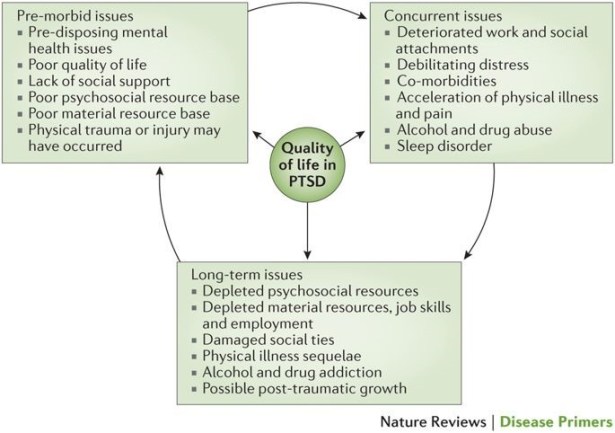
There is a 75% to 90% increase in risk of a low quality of life including isolation, drinking, depression, suicidal ideation, and poor coping skills with basic life stressors are obstacles that veterans have to endure and overcome to live a normal life. Several studies report that female veterans with insomnia and probable PTSD had poorer sleep quality than veterans with insomnia alone. Combat veterans and their exposure to war zones endure mental trauma but women have the added possible sexual trauma in combat areas. For the young veterans who deal with sleep disturbances the cost is great both mentally and physically over their lifetime. They can be utilized for future studies for treatments options and data to reduce risk for veterans in the future.
There are limited treatments for PTSD associated sleep disturbances. One possible option is explored in auricular acupuncture as described in Heather King et al. (582-590) being successful when studied in a small group of veterans with PTSD. Acupuncture increases endogenous opioid levels and melatonin and during interaction to promote sleep. There were no negative comments when the study was concluded. With a ninety five percent approval rating among those who were question one participant replied, “My sleep significantly improved due to acupuncture. I felt better rested and helped me concentrate on my days and I performed better on my daily activities….(Heather King et al. pp.587). Although it is a primary study of a non-medication form of treatment. Although there are some with other severe issues that require medication and unclear if this treatment would work for them along with medication and psychiatric intervention.
Medication is the first option given to veterans who suffer from PTSD and sleep disorders. Risperidone which is an antipsychotic drug may be prescribed for the more severe cases of PTSD. In the study conducted and reported by Daniella David et al. (489-491) nightmares shifted toward less trauma-replicating allowing better sleep. It did not cure or allow the participant to sleep consistently but may have eased some of the bad dreams decreasing the nighttime awakenings.
There are many variables and case by case issues with treatments among the veterans with PTSD and sleep disorders. There may be more than one treatment that is required to alleviate the symptoms they experience. All require therapy and some need a sleep study to determine if a form of life support is needed. Medication is usually administered for a diagnosis of depression, hallucinations, suicidal ideation or insomnia. It is a combination of treatments to assist the veteran in being functional in life to assume the pursuit of the “American Dream.” Our veterans deserve to live a full, well adjusted and happy life when they return home from their duty in the service. Not all of us can volunteer for such a duty or aren’t as brave as the soldiers that continue to be part of this elite group of men and women. My husband is a combat veteran and has been diagnosed with PTSD once he returned home. Sleep is definitely a variable for him and at times it can affect me as well. Medication is a daily requirement and even so there are still effects that cannot be escaped or cured.
New studies need to be conducted to explore alternative options for future veterans and those who still suffer from PTSD and sleep disorders. Winding down at the end of the day by taking a bath or avoiding coffee may help but the psychological trauma is what is most disruptive. The environment where they sleep should also be appropriate to feel comfortable and safe. Short naps throughout the day may keep from feeling so exhausted at the end of the day. The mental condition will never cease to exist and can be developed in more than this specific scenario. Sleep may be the only escape and unsuccessful attempts and nightmares create more issues that contribute to self-medicating such as drugs, alcohol or suicide.
The Department of Veterans Affairs offers services and assistance of no- cost to veterans for those who seek help to resolve issues they may be suffering from. Accounts from veterans willing to share can be viewed at Meet the Connection website where Justin states at a certain point he walked into a VA and stated, “I need help immediately,” (maketheconnection.net). He speaks of his life in chaos with relationships falling apart and suicidal ideation. Those who are willing to accept help and admit there is a problem can seek it through the VA system. Many go to individual and group therapy or may record their traumatic accounts and journal about their feelings. Their strength and resilience in and out of the service is part of what makes America great.
Work Cited
David, Daniella, et al. “Adjunctive Risperidone Treatment and Sleep Symptoms in Combat Veterans with Chronic PTSD.” Depression and Anxiety (1091-4269), vol. 23, no. 8, Dec. 2006, pp. 489-491
Hughes, Jaime et al. “Insomnia and Symptoms of Post-Traumatic Stress Disorder Among Women Veterans.” Behavioral Sleep Medicine, vol. 11, no. 4, Sept. 2013, pp. 258-274
King, Heather C., et al. “Auricular Acupuncture for Sleep Disturbances in Veterans with Post-Traumatic Stress Disorder. A Feasibility Study. “Military Medicine, vol. 180, no. 5, May 2015, pp. 582-590
Straus, Laura D., “Sleep and Variability in Military-Related PTSD: A Comparison to Primary Insomnia and Healthy Controls.” Journal of Traumatic Stress, vol. 28, no. 1, Feb. 2015, pp. 8-16.
Van Liempt, Saskia, et al. “Impact of Impaired Sleep on the Development of PTSD Symptoms in Combat Veterans: A Prospective Longitudinal Cohort Study.” Depression and Anxiety (1091-4269), vol. 30, no. 5, May 2013, pp. 469-474.
https://maketheconnection.net/symptoms/trouble-sleeping Accessed 10/2018
Photo Credits
Twitter.com/VA_PTSD-Info
Eopssleep.com/2014/09/11/ptsd
Medicalexpress.com/news/2018-3
Green, Peter S. Post-Traumatic Sleep Disorders Are the New PTSD. Published 10/19/2015
Nature Reviews/Disease Primers PTSD. Published 8,Oct 2015 Rachel Yehuda et al.
